The Spread of the Tick-Borne Alpha-Gal Syndrome Foreshadows the Future of Diseases Influenced by Climate Change
Climate change is exacerbating the spread of diseases.
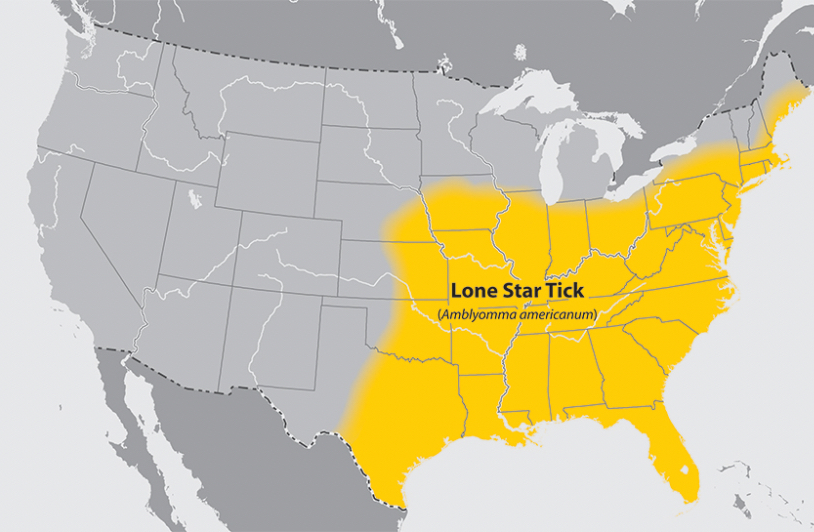
The lone star tick is a prime example of this. The species is taking advantage of climbing temperatures by widening its territory in the southeastern and southcentral U.S. and expanding as far as the northern U.S. and eastern Canada. More people are being affected by the pathogen it carries, which results in a condition called alpha-gal syndrome (AGS) and causes an allergy to meat and dairy.

During the summer of 2022, the CDC issued a report explaining that the number of people diagnosed with AGS spiked by 41% between 2017 and 2021. The impact of climate change on the spread of AGS foreshadows future patterns of other emerging and expanding health threats to humans. And ticks aren’t the only vector.
“The evidence is overwhelming that climate change is one of the main drivers of emerging infectious diseases,” said Rick Ostfeld, a distinguished senior scientist at the Cary Institute of Ecosystem Studies in New York.
In a 2022 study, Erik Franklin, a Ph.D. and associate research professor at University of Hawaii at Mānoa, found that 58% of infectious diseases have at some point been aggravated by climate hazards.
This includes a host of diseases that can be spread by ticks, mosquitoes, animals, fungi and water. For example, increased precipitation during winter and spring in Colorado has contributed to a rising mosquito population, heightening the risk of exposure to West Nile; and rising temperatures have enabled the fungus Coccidioides, known to live in hot and dry conditions in the southwestern U.S., to spread to the Pacific Northwest, increasing the geographic range of risk for Valley fever.
Franklin says that as the planet warms, disease-carrying pests like ticks, mosquitoes and fleas are able to expand their habitats. Longer periods of warmer temperatures create a longer active season, allowing them more time to travel and carry pathogens into new areas.
These developments significantly increase the risk of contact between pathogens and humans. They also render physicians unprepared for not only recognizing new or lesser-known illness from these spreading pathogens but also for treating them. This unpreparedness is evident in how AGS has been dealt with so far.
The lone star tick was pushed out of its original habitat, the Midwest, largely due to tree clearing and land development. The species had retreated to the southeastern and southcentral U.S. But climate change has helped create the conditions for this species to expand back to the Midwest and farther, into areas of Canada. This spreading occurs through the ticks’ own migration as well as by its attachment onto traveling mammals, like white-tailed deer. Many of the mammal species that pests latch onto are also experiencing population and habit increases linked to climate change, further adding to the risk of pest-borne pathogens.
Katie Cahoj, in southcentral Missouri, always had a freezer fully stocked with beef by her cattlefarming father, until July 2020, when she was diagnosed with AGS.
No treatment or cure is currently available for the syndrome. A survey carried out by the CDC on healthcare providers’ awareness of AGS revealed that many had never heard of it or didn’t know how to treat it.
Cahoj was diagnosed by her primary care physician. She was able to advise multiple friends, who had undiagnosed AGS at the time, to suggest the possibility of AGS to their physicians.
“After diagnosis you’re really left to figure it out on your own,” Cahoj said. She wrote a cookbook, “An Alpha-Gal Cooks,” six months after her diagnosis because there were no available, helpful resources for her at the time.
Habitat destruction has also contributed to the spread of lone star ticks. Climate change can cause severe weather events, like droughts or storms, and long-term increases or decreases in temperature, which harm habitats and impact their biodiversity.
The CDC issued a report in 2020 that explains that climate change has affected the geographic distribution and range of other insects and pests, like mosquitoes carrying Lyme disease, Zika, West Nile and dengue.
“Humans overcome disease by exposure,” says Ostfeld. When human populations that were entirely unexposed to a certain pathogen, historically not present in their geographic range, become exposed, “very rapid epidemics” can occur, he says.
But it goes both ways. Human populations are also shifting their locations due to climate change.
Climate hazards, like weather events that have been strengthened by climate change, cause people to move out of their normal home areas and go to areas where they’re more susceptible to pathogens that they aren’t used to, says Franklin. He explains that this migration also increases the chances that humans will be exposed to pathogens that have been strengthened by climate change in certain regions.
In terms of keeping up with emerging environmental threats, experts agree that the responsibility of identifying conditions should rest on a patient’s first line of defense: the general practitioner.
Building off of what already exists instead of creating an “emerging environmental conditions” specialist field is essential to beginning to create equal, global care for environmental threats.
“If we only have specialists then only the privileged will be able to benefit from that,” says Ostfeld. The impact of climate change on diseases is already spread disproportionately among humans.
Certain, less developed areas may have fewer degrees of separation from the environment, so people there are more vulnerable to and will be more affected by any changes. Infrastructure, like pipes or electricity, makes an area more tolerant to climate hazards. A simple example of this is air conditioning and TV: a person will spend more time in the comfortable temperature of their home watching TV, rather than going outside, decreasing the chances that they are exposed to pathogens that have been enhanced by climate change.
“A very critical piece of the puzzle that’s missing right now is surveillance,” says Jennifer Platt, a Ph.D. and co-founder and director of Tick-borne Diseases United based in North Carolina. The non-profit is dedicated to helping diagnose and treat tick-borne diseases, the prevention of such diseases as well as conducting research and educating about these diseases. She discusses how tracking the spread of diseases will help identify “when to raise a red flag.”
Many states in the southeast and central U.S. encourage the reporting of positive AGS cases to their Department of Health, however the CDC only requires voluntary reporting. Thus, many states are forced to do estimates. This makes it difficult to track the syndrome’s impact and distribution. However, in some states, like Rhode Island, providers are required to report positive tick-borne laboratory results, including but not limited to AGS.
Improved surveillance and tracking of emerging conditions exacerbated by climate change could be crucial to creating an efficient system that addresses environmental health threats, experts say. This type of tool would help spread awareness of conditions globally and provide aid to the affected regions.
Franklin and his team created an online database that enables practitioners to track the effects of climate on human infectious diseases. He says that healthcare providers should be aware of how things are going to be changing and expanding into areas that they historically haven’t been.
“We’re always facing new realities,” Ostfeld says. Many experts want to see the medical practice become more adaptive and openminded, as practitioners will likely encounter an increasing number of conditions that they haven’t seen before, which have rapidly spread due to climate change.
Platt explains that it’s essential for doctors to listen to their patients when they are describing their symptoms, and to not stick to the rigid boundaries of what they already know.
In terms of AGS, these boundaries have caused patients much distress—when their symptoms don’t line up with what their physician knows, and they leave the office confused about their condition.
From the patient’s side, Cahoj explains the importance of advocating for your symptoms, because sometimes the practitioner may not understand or be willing to put in the time to do more research on new conditions.
The CDC’s Building Resilience Against Climate Effects (BRACE) outlines steps that can be taken to help communities prepare for the health impacts of climate change. The acronym is aimed at healthcare officials.
The implementation of new regulations and systems is well-known to be a slow process. Platt explains how social media helped to amplify the voices of people with AGS. The public can continue to create conversation and share their stories relating to other emerging or new environmental health threats, as this might be the most effective system for spreading awareness at the moment.
“Everything that we know about allergies isn’t followed by alpha-gal,” says Platt. Open collaboration and communication between patients, providers and the public are paramount to keeping up with lesser-known emerging and expanding diseases.




